Can Cognitive Behavioral Therapy Treat Physical Intimacy Issues? Here’s What the Evidence Says
Can cognitive behavioral therapy treat physical intimacy challenges? Yes — and the research backs it up strongly.
CBT can help with a wide range of intimacy and sexual health issues, including:
- Low sexual desire (HSDD/SIAD)
- Performance anxiety
- Pain during sex (dyspareunia, vaginismus)
- Difficulty with arousal or orgasm
- Negative body image affecting intimacy
- Relationship communication barriers
Physical intimacy isn’t just a body issue. It’s deeply connected to how you think, feel, and relate to your partner. Anxiety, shame, fear of failure, and negative self-talk can all create real barriers in the bedroom — even when there’s nothing physically wrong.
That’s exactly where CBT comes in. It works by identifying and changing the thought patterns and behaviors that get in the way of connection and pleasure. And unlike some therapies that dig into your past for years, CBT is present-focused — meaning you start building new skills quickly.
Clinical research shows up to a 66% improvement in sexual performance after just 12 weeks of CBT. Studies also show significant, lasting improvements in desire, arousal, comfort, and satisfaction — with benefits that hold up at 6-month follow-ups.
I’m Dr. Neil Cannon, an AASECT Certified Sex Therapist with a Doctorate in Human Sexuality and decades of experience helping individuals and couples explore can cognitive behavioral therapy treat physical intimacy challenges in a safe, research-informed setting. In this guide, I’ll walk you through exactly how CBT works for intimacy — the techniques, the evidence, and how to know if it’s right for you.
Can cognitive behavioral therapy treat physical intimacy terms explained:
Understanding How Cognitive Behavioral Therapy Treats Physical Intimacy
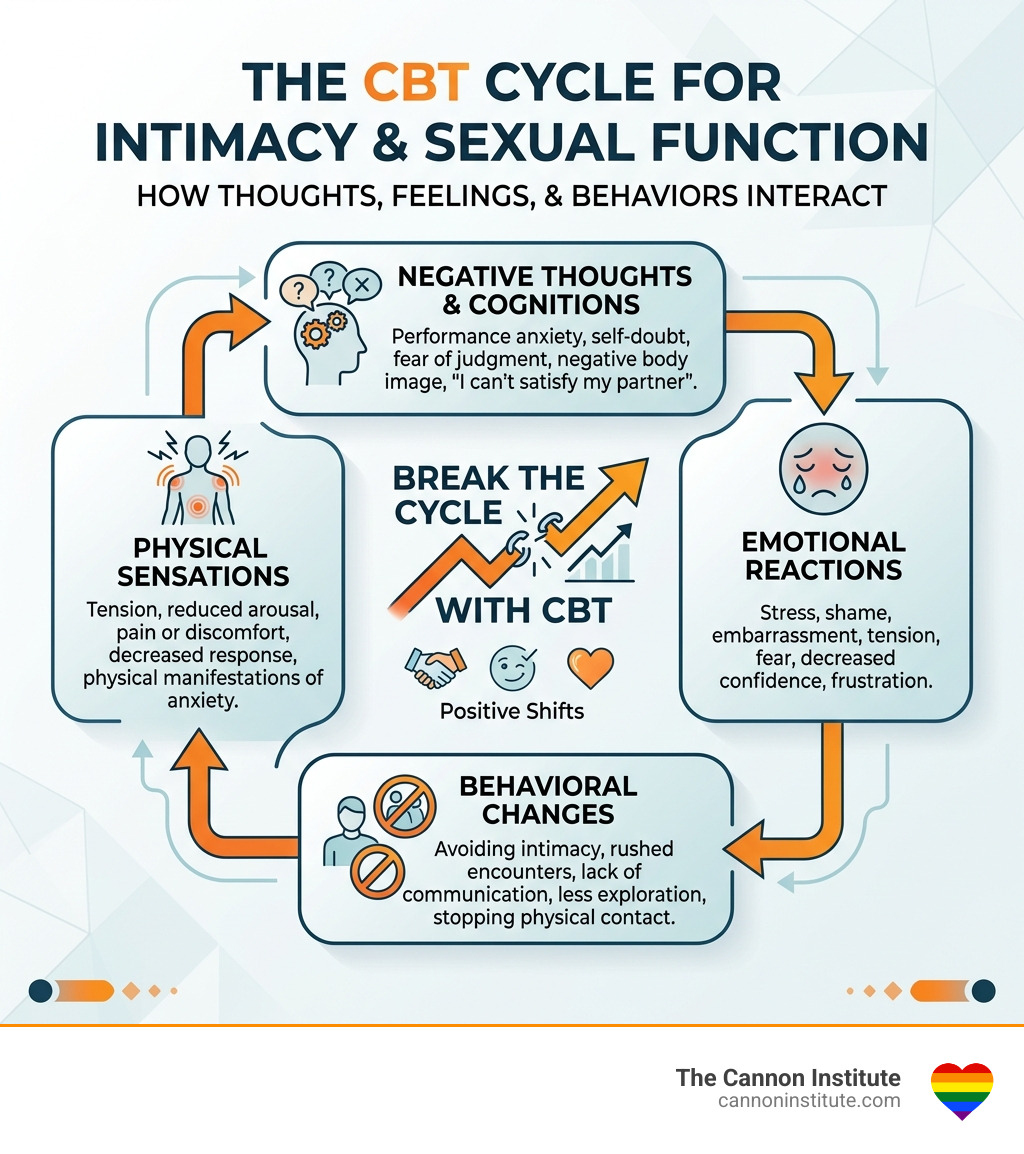
At its core, Cognitive Behavioral Therapy (CBT) is based on the idea that our thoughts (cognitions), feelings, and actions (behaviors) are all interconnected. When it comes to the bedroom, a single negative thought like “I’m not going to be able to perform” can trigger physical anxiety, which then leads to avoidance or difficulty with arousal. This creates a self-fulfilling prophecy that reinforces the original negative thought.
In our practice, we use cognitive restructuring to help clients identify these “unhelpful” thought patterns. Instead of letting a catastrophic thought run wild, we look at the evidence. Is it true that your partner will leave you if things aren’t “perfect” tonight? Usually, the answer is no. By reframing these thoughts, we lower the emotional temperature, making physical connection feel possible again.
CBT is also a present-focused approach. While your history matters, we focus on the “here and now”—the specific triggers and patterns happening today. We often use the fear-avoidance model to explain why intimacy has become stressful. If sex has been painful or anxiety-inducing in the past, your brain naturally tries to protect you by avoiding it. CBT helps retrain the brain to see intimacy as a safe, pleasurable experience rather than a threat.
For those looking for a deeper dive into the clinical side, Cognitive Behavioral Therapy for Sexual Dysfunctions in Women provides extensive data on how these interventions specifically target female sexual health. If you feel like your challenges are more personal or internal, more info about individual therapy can help you understand how one-on-one sessions build the foundation for better intimacy.
Can cognitive behavioral therapy treat physical intimacy issues like performance anxiety?
Performance anxiety is one of the most common reasons people ask, “can cognitive behavioral therapy treat physical intimacy?” It acts like a “spectator” in the room—instead of feeling the sensations of touch, you are watching yourself and worrying about the outcome.
The good news? 85% of people using systematic desensitization (a key CBT technique) experience significant improvement in sexual performance anxiety. This process involves gradually exposing yourself to intimate situations in a low-pressure way, retraining your nervous system to stay relaxed.
We also teach practical “in-the-moment” tools to interrupt the anxiety loop:
- 4-7-8 Breathing: Inhale for 4 seconds, hold for 7, and exhale for 8. This physically forces your nervous system out of “fight or flight” mode.
- 5-4-3-2-1 Grounding: Name 5 things you see, 4 you can touch, 3 you hear, 2 you smell, and 1 you can taste. This pulls your mind out of your “head” and back into your body.
By mastering these techniques, you stop the cortisol spike that kills arousal. You can learn more about how CBT improves mental well-being and sexual function to see how these mental shifts create physical results.
Addressing Female Sexual Dysfunction with CBT
For women, sexual challenges often fall into categories like Hypoactive Sexual Desire Disorder (HSDD), Sexual Interest/Arousal Disorder (SIAD), or Orgasmic Disorder (FOD). CBT is highly effective for these because it addresses the psychological “brakes” that prevent desire.
One of the most well-established CBT treatments is Directed Masturbation (DM) for primary anorgasmia (never having had an orgasm). Research shows this is one of the most successful interventions available, helping women understand their own bodies and what feels good without the pressure of a partner present.
For conditions like vaginismus (involuntary tightening of the vaginal muscles), CBT targets the fear of pain. By combining cognitive work with gradual exposure, women can regain a sense of control over their physical responses.
| Outcome Category | CBT Effectiveness Improvement |
|---|---|
| Sexual Desire | Significant increase in interest and mental “space” for sex |
| Arousal | Reduced anxiety allows for better blood flow and lubrication |
| Orgasm | Higher consistency and satisfaction through body awareness |
| Comfort/Pain | Significant reduction in “pain catastrophizing” and physical tension |
CBT Techniques for Improving Sexual Function and Desire
When we work with couples or individuals, we don’t just talk; we use specific, evidence-based exercises. One of the “gold standards” in sex therapy is Sensate Focus. Developed by Masters and Johnson, this is a series of non-demand touch exercises.
The goal isn’t “performance” or even orgasm; it’s simply to notice sensation. By taking the pressure of “completion” off the table, the body can finally relax enough to actually enjoy the touch. This is a form of exposure therapy where we slowly reintroduce physical connection in a way that feels safe.
We also spend a lot of time on body image. If you are constantly thinking about how your stomach looks or how much you weigh while you’re intimate, you aren’t actually present for the pleasure. CBT helps challenge those distorted beliefs and replaces them with a more compassionate, realistic view of your body.

If you’re ready to move beyond self-help, our professional sex therapy services offer a structured way to apply these techniques to your specific situation.
Can cognitive behavioral therapy treat physical intimacy by improving communication?
Intimacy is a team sport. Often, the “dysfunction” isn’t in one person—it’s in the communication between them. Cognitive Behavioral Couple Therapy (CBCT) focuses on interpersonal emotion regulation. This means learning how to help your partner feel safe and how to express your own needs without fear of judgment.
In a recent study on SIAD, couples who underwent a manualized CBCT program showed massive improvements. Women reported a significant increase in dyadic desire (desire specifically for their partner), and both partners saw a major drop in sexual distress.
Improving communication is often the path to stronger relationships. When you can say, “I really like it when you do this,” or “I’m feeling a bit anxious tonight, can we just cuddle?” the pressure disappears, and true intimacy can grow. You can find more details on the feasibility of CBT for SIAD and how it helps couples reconnect.
Targeted Interventions for Sexual Pain
Pain during sex—whether it’s dyspareunia or Provoked Vestibulodynia (PVD)—is incredibly common but often goes untreated. Many women think they just have to “deal with it,” which leads to pain catastrophizing (worrying that every touch will hurt).
CBT treats sexual pain by:
- Breaking the Pain-Anxiety Cycle: Teaching relaxation techniques to prevent the pelvic floor from clenching in anticipation of pain.
- Cognitive Reframing: Changing the internal dialogue from “This is going to hurt” to “I am in control, and we can stop whenever I want.”
- Mindfulness: Helping you stay present with pleasurable sensations rather than scanning for pain.
Understanding what is intimacy and how to reclaim it is the first step toward moving past the fear of pain and back toward the joy of connection.
CBT vs. Medical Treatments: Which is More Effective?
This is a question we hear often: “Should I just take a pill?”
Medical treatments like lidocaine, sildenafil (Viagra), or bupropion can provide rapid physiological relief. They are great for “jumping-starting” the system. However, they don’t address the underlying psychological or relational issues. If you take a pill for arousal but still feel anxious about your body or angry at your partner, the pill can only do so much.
Research shows that while medical treatments offer speed, CBT offers durability. In direct comparisons, CBT often provides broader improvements in overall sexual function and relationship satisfaction. This is because CBT teaches you skills that you keep for life, whereas medication only works as long as you take it.
Check out the comparative effectiveness of CBT vs medical treatment for a deeper look at the data.
Long-Term Durability and Sustained Benefits
One of the most impressive statistics in sex therapy research is the 18.08-point increase in Female Sexual Quotient (FSQQ) scores for those using CBT, compared to almost no change in control groups.
More importantly, these benefits last. At 6-month follow-up appointments, most people who completed a CBT program for intimacy reported that their improvements were maintained or even grew. This is because you’ve learned relapse prevention. You know what your triggers are, you know how to talk to your partner, and you have a “toolbox” of techniques to use if things get off track.
Moving toward shedding shame and embracing confidence isn’t just a temporary fix—it’s a lifestyle change.
When to Use a Combined CBT-Medical Approach
Sometimes, the best answer to “can cognitive behavioral therapy treat physical intimacy” is “Yes, especially when combined with medical support.”
For example, a man dealing with erectile dysfunction might use medication to regain confidence in his physical response while simultaneously using CBT to address the performance anxiety that caused the issue in the first place. This synergistic approach offers the “best of both worlds”: rapid symptom relief and long-term psychological healing.
We often recommend this for:
- Severe sexual pain (medical treatment for tissue healing + CBT for fear)
- Erectile dysfunction with high anxiety
- Complex cases of HSDD where hormonal issues and relationship stress overlap
Our approach to erectile dysfunction sex therapy often looks at these holistic, combined paths.
Frequently Asked Questions about CBT and Intimacy
How long does it take to see results with CBT for sex?
Most clinical protocols, like the ones we use at The Cannon Institute, show significant results within a 12-week timeline. While every individual is different, many people report a 66% improvement in their primary concerns within those first three months. Consistency is key—attending weekly sessions and following through with “home play” (our term for homework) makes a massive difference. If you’re looking to boost sexual confidence, starting today can lead to a very different life just a few months from now.
Is CBT better than medication for low libido?
For many women with HSDD/SIAD, CBT is actually more effective than medication because low desire is so often tied to stress, relationship dynamics, and mental “clutter.” While medication can help with the physiological side, CBT addresses the reasons why the desire was lost in the first place. It provides a more comprehensive outcome that includes better communication and emotional closeness.
Can cognitive behavioral therapy treat physical intimacy for couples?
Absolutely. In fact, for many issues like SIAD or PVD, couple-based CBT is the preferred method. When both partners are involved in the exercises and the communication training, the “burden” of the dysfunction is lifted off one person’s shoulders. You work together as a team to rediscover pleasure. If you’re curious about this, more info about relationship therapy can explain how we bring both partners into the healing process.
Conclusion
At The Cannon Institute in Cherry Creek, Denver, we believe that a fulfilling intimate life is within reach for everyone. Led by Dr. Neil Cannon, our practice is dedicated to providing a research-based, intentional process that goes beyond simple talk therapy.
We offer immediate, targeted interventions designed for the unique needs of diverse individuals and couples in Colorado. Whether you are struggling with pain, anxiety, or a lack of desire, we provide the tools for sustainable change and a renewed sense of hope. You don’t have to navigate these challenges alone.
Ready to see how “Mind Over Matter” can change your relationship? Start your journey with sex therapy today and discover the path to a more connected, pleasurable life.













